Best Practices for Maintaining Sample Integrity During Drug Test Collection

A drug test is only as reliable as the sample behind it. When collection procedures break down, even the best test can produce a result people question. This guide covers how to protect sample integrity during drug test collection, what collectors should watch for, and which simple controls help prevent mix-ups, contamination, dilution, and tampering.
What does sample integrity mean in drug test collection?
Sample integrity means the urine specimen came from the correct donor, stayed in the proper container, and reached testing without tampering, substitution, or contamination. Put simply, the sample has to remain valid from collection through testing or transfer.
Most collection issues come down to a short list: incorrect donor identification, poor labeling, temperature problems, delayed handling, adulteration, leakage, and weak documentation. Control those points, and you protect the result while reducing disputes later.
Why does sample integrity matter so much?
Rapid drug tests deliver quick answers, but speed does not make process less important. If a specimen sits too long, arrives at the wrong temperature, or changes hands without documentation, confidence in the result drops. That creates risk for employers, clinics, treatment programs, and families.
Sample integrity matters for another reason: donors trying to avoid detection usually target the collection process, not the test strip. They may attempt dilution, substitution, synthetic urine, adulterants, or even simple label confusion. A solid collection routine stops many of those tactics before testing begins.
Start with the collection area
Control access and remove easy tampering tools
The collection area should be quiet, clean, and stripped down to essentials. Limit traffic in and out. Remove soaps, cleaning agents, open containers, and loose items near the collection point that could be used to alter the specimen. If policy allows, secure water sources or closely monitor access during the collection window.
This matters more than it may seem. A cluttered restroom or collection room gives a donor more opportunities to hide items, add water, or switch containers. A controlled space cuts that risk immediately.
Keep supplies ready before the donor arrives
Collectors should have supplies prepared before collection starts. That includes sealed cups, gloves, labels, forms, and any transfer tools. When staff start hunting for supplies after the specimen is produced, control over the process weakens.
- Use sealed, clean specimen cups
- Keep labels and forms within reach
- Wear fresh gloves for each collection
- Prepare temperature review and timing steps in advance
Verify donor identity before collection
One of the simplest mistakes is also one of the most damaging: collecting from the wrong person or labeling the right sample with the wrong name. Verify identity before handing over the cup. Match the donor to the order, roster, or ID required by policy.
Then label clearly and immediately. Do not place unlabeled cups on a counter and plan to sort them out later. That is how errors happen. The safest approach is straightforward: one donor, one cup, one label, one documented handoff.
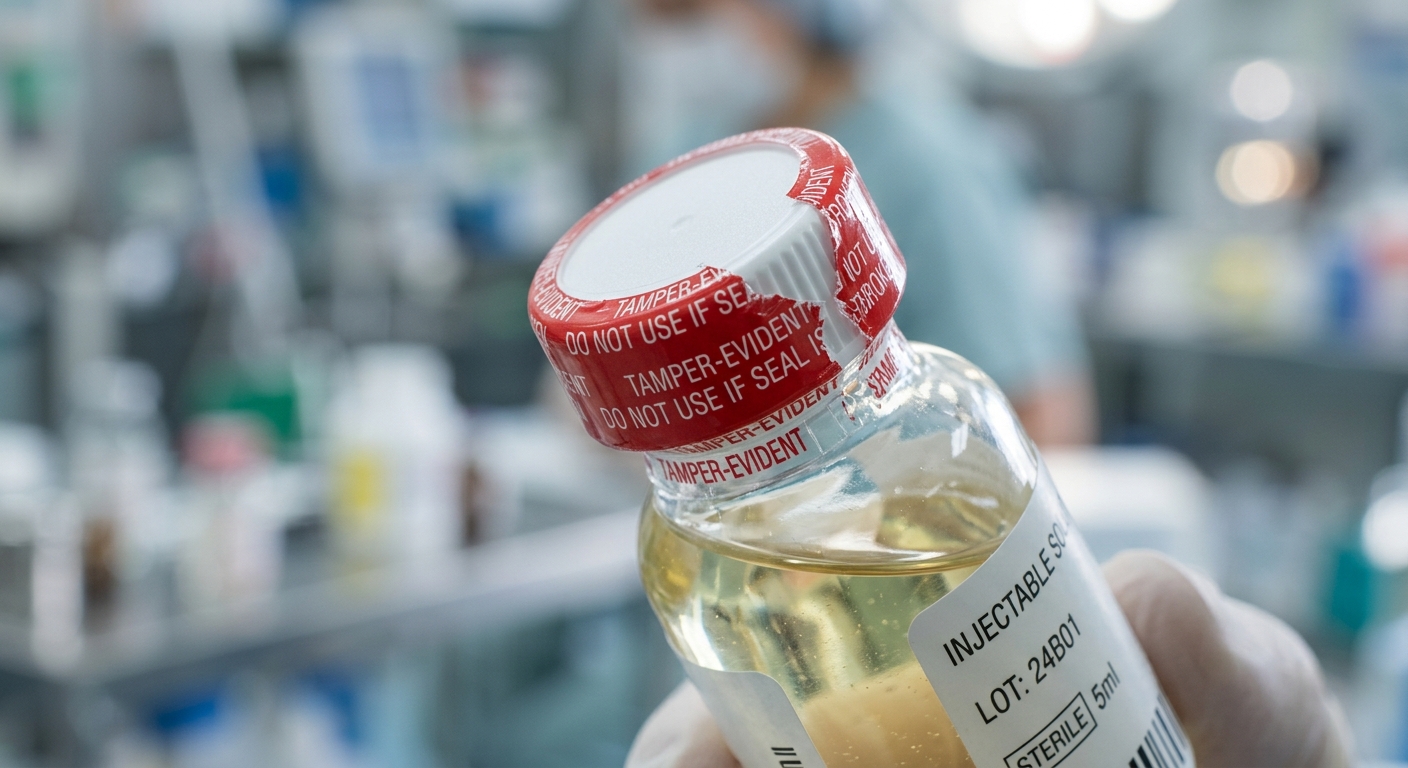
Use containers that support validity checks
The collection container matters. A plain cup can hold urine, but a purpose-built specimen cup adds control. Cups with temperature strips help staff confirm freshness right after collection. Tamper-evident and leak-resistant designs help prevent accidental loss and reduce questions about handling.
When samples need to be transferred for additional testing, closed-transfer options reduce spills and minimize contact points. That is one reason many professional programs use cups or containers designed for safer specimen handling, especially when follow-up testing is part of the process.
Check specimen temperature right away
Temperature is one of the fastest and most useful validity indicators. Fresh urine should fall within an expected range shortly after collection. If the reading is outside that range, staff should treat the specimen as questionable and follow policy for recollection or escalation.
The key is timing. A late temperature check tells you very little because urine cools quickly. Cups with built-in temperature strips make this easier, allowing the collector to review the strip within minutes while the sample is still fresh.
Watch for signs of dilution, substitution, or adulteration
Start with the basic physical signs. Does the specimen look unusually clear? Is the volume too low or oddly high for the situation? Is there an unusual smell, color, or foam pattern? None of those signs proves tampering by itself, but each one deserves attention.
For stronger control, many programs use tests or cups with specimen validity checks built in. Adulteration checks such as pH, creatinine, and specific gravity can flag samples that appear normal at first glance but fail basic chemistry review. That extra layer is especially useful in workplace, treatment, and probation settings where sample validity may be challenged.
Limit handling and shorten the timeline
Every extra handoff creates another chance for error. Every delay creates another chance for degradation, confusion, or dispute. A strong collection process should move in a straight line: collect, inspect, label, document, test or transfer, and secure.
If the sample needs to be transferred to tubes or another testing step, use a method that reduces open pouring and surface exposure. Closed-system transfer tools help lower spill risk and keep the specimen contained. That protects both the sample and the person handling it.
Document each step with clean chain of custody
Chain of custody may sound formal, but the goal is simple. You need a clear record of who collected the specimen, when collection happened, what was observed, and who handled the sample afterward. If a result is questioned, that record becomes the foundation of your response.
Good documentation should include:
- Donor identification details required by policy
- Date and time of collection
- Temperature check result
- Any unusual observations
- Collector name or initials
- Transfer, storage, or shipping details if used
Keep entries clear and immediate. Do not rely on memory at the end of the day.
Train collectors to follow the same routine every time
Even the best protocol fails if each staff member runs it differently. A repeatable routine protects integrity better than a complicated one. Staff should know the order of steps, the timing for temperature review, the signs of tampering, and exactly when labeling and documentation must happen.
Consistency also improves fairness. Donors notice when one person goes through a stricter process than another. A standard workflow reduces complaints and provides stronger support if a result leads to action.
What equipment helps protect sample integrity?
The right supplies do not replace sound procedure, but they do make it easier to maintain control. In day-to-day collection settings, a few tools make the biggest difference.
- Specimen cups with temperature strips: allow fast freshness checks
- Tamper-evident collection cups: reduce disputes after collection
- Adulteration-enabled cups or dip cards: help flag diluted or altered samples
- Vacuum transfer containers or cups: reduce spills and contamination during transfer
- Nitrile gloves: support clean handling between collections
For example, programs that need built-in checks often prefer cups that combine temperature review with adulteration controls. Programs that separate on-site screening from later specimen transfer often benefit from vacuum-style collection tools because they keep handling cleaner and more controlled.
Common mistakes that weaken a drug test sample
Most integrity failures do not come from the chemistry. They come from rushed collection habits. Watch for these mistakes:
- Handing out unlabeled cups
- Checking temperature too late
- Leaving the sample unattended
- Using the wrong donor paperwork
- Allowing clutter or water access near collection
- Ignoring unusual specimen appearance
- Writing notes after the fact instead of in real time
Any one of these can seem minor. Together, they create serious doubt around the result.
When should a collector question the sample?
A collector should pause and review policy any time the specimen raises a validity concern. Common triggers include temperature outside the expected range, unusual color, suspiciously clear urine, low volume, delayed handoff, or donor behavior that suggests substitution.
The right response is not guesswork. Follow written policy, document what you observed, and move to recollection or confirmation steps when required. A calm, documented response protects everyone better than an argument in the collection room.
FAQ
How fast should temperature be checked after urine collection?
It should be checked within minutes of collection. A delayed check loses value because fresh urine cools quickly, which weakens one of the simplest validity markers.
Can a rapid drug test still be useful if the sample integrity is questionable?
No result should stand on a weak specimen. If integrity is in doubt, the right step is to follow policy for recollection, adulteration review, or lab confirmation.
What is the easiest way to improve sample integrity right away?
Use the same standard process every time: verify identity, use a temperature-strip cup, label at the point of collection, document each handoff, and never leave the sample unattended.
Conclusion
Maintaining sample integrity during drug test collection comes down to control, speed, and consistency. A clean collection area, prompt temperature review, accurate labeling, validity checks, and a clear chain of custody prevent most avoidable problems. If you need collection tools that support those steps in real-world settings, 12 Panel Now is a practical place to start.
This guide was written by the team at 12 Panel Now, suppliers of rapid drug testing and specimen collection products since their founding.