Oral Fluid vs. Urine Drug Testing: A Comparative Analysis
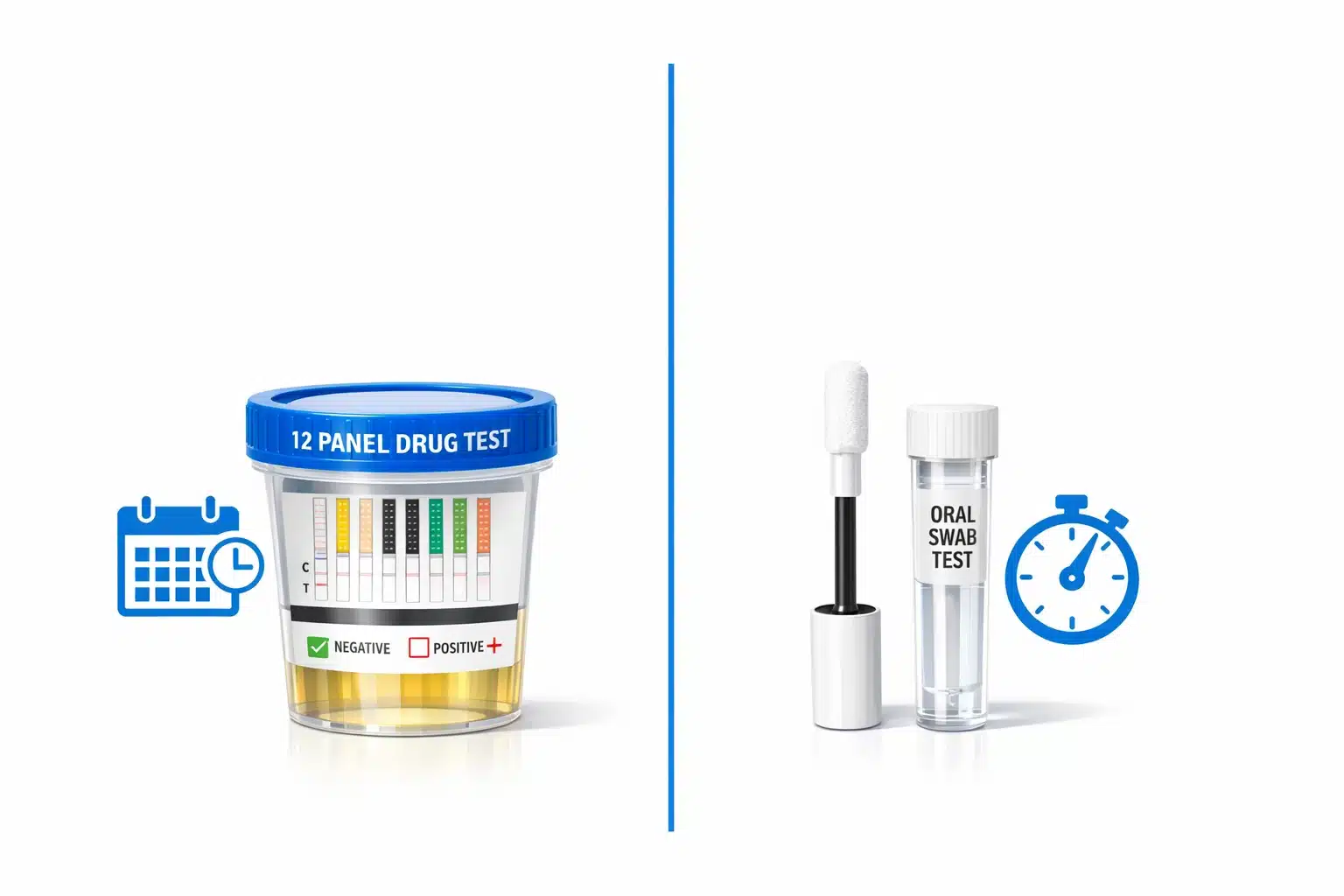
If you are managing a workplace testing program in 2026, you are likely feeling the tension between two competing priorities: the absolute necessity of workplace safety and the relentless pressure to accelerate your “speed to hire.”
For decades, the 10-panel urine screen has been the undisputed gold standard for employee drug testing. However, a massive shift in regulatory frameworks—spearheaded by the Department of Transportation’s (DOT) 2024 Final Rule—and a multi-million-dollar surge in the drug test adulteration industry have forced decision-makers to reevaluate their protocols. Today, selecting between oral fluid and urine testing is no longer a simple matter of preference; it is a strategic decision that impacts your recruitment ROI, your legal liability, and your operational compliance.
To make the right choice for your organization, you need to look past surface-level pros and cons. You need a data-driven decision matrix.

Defining the Methods: The Accuracy Paradox and Detection Windows
When evaluating testing solutions, the first question employers ask is typically, “Which test is more accurate?” The answer depends entirely on what you are trying to measure.
Urine and oral fluid are both highly reliable—especially when utilizing FDA-approved and CLIA-waived point-of-care testing (POCT) supplies—but they tell two fundamentally different stories about a candidate’s substance use.
In a definitive 1,500-sample pair study comparing the two methods, urine was found to be 7.4 times more likely to detect substances overall, yielding a 3.7% positivity rate compared to oral fluid’s 0.5% (Casolin, PMC4986628). This staggering difference isn’t due to faulty saliva tests; it is a direct result of detection windows.
Urine captures a much wider historical window of substance use (typically 3 to 30 days, depending on the substance). Oral fluid, on the other hand, is a real-time indicator. While some outlier claims suggest up to a 4-day window for saliva, the established clinical consensus places the oral fluid detection window closer to 24 to 48 hours.

Here lies the “Accuracy Paradox”: While urine offers a broader historical view, it is highly susceptible to tampering. The oral fluid window is shorter, but its adulteration rate is near 0% because the collection is 100% observed.
Navigating the DOT Final Rule and Operational Compliance
The landscape fundamentally shifted with the implementation of the DOT’s 2024 Final Rule (49 CFR Part 40), which officially mandated oral fluid as an acceptable testing method for transportation and safety-sensitive workplaces. This wasn’t just a minor regulatory update; it was a green light for employers to overhaul their logistics.
Why the push from regulators? Flexibility and risk mitigation.
Under the current rules, employers must explicitly utilize “Qualified Oral Fluid Collectors” and “Urine Collectors.” The operational brilliance of the oral fluid option is that it dramatically reduces “refusal to test” scenarios resulting from shy bladder syndrome (paruresis). Furthermore, it eliminates the expensive logistical requirement of sending employees to off-site, private collection facilities with secured water sources.

By keeping the collection in-house with highly reliable, fast-acting screening supplies, companies can screen candidates immediately post-interview. For high-volume employers, this operational pivot saves thousands of dollars in facility fees and significantly shortens the onboarding runway.
The Science of Detection: Parent Compounds, Metabolites, and the “Edibles” Nuance
To truly understand which test your organization needs, you must understand how these tests interact with human biology.
Drug tests look for specific chemical signatures. Urine tests are designed to detect metabolites—the chemical byproducts created after the liver breaks down a drug. Oral fluid tests, conversely, look for the parent compound—the actual un-metabolized drug itself lingering in the body.
This distinction is mission-critical when building your drug testing policy, particularly concerning THC in today’s environment.
Because oral fluid looks for the parent compound, it primarily detects THC from residual smoke or resin coating the oral cavity. Therefore, individuals who consume cannabis via edibles will clear an oral fluid test significantly faster—often in less than 12 hours—because there is no smoke residue in the mouth (NIH-PMC9890870). A urine test, hunting for the metabolized byproduct (THC-COOH), will catch that edible use days or even weeks later.
Similarly, drugs like phentermine (a commonly prescribed weight-loss medication that can trigger amphetamine panels) will present differently across the two tests based on how quickly the parent compound is metabolized versus how long the metabolites are excreted.

The “Cheating” Reality Check: Why Adulteration Fails
We cannot discuss MOFU testing strategies without addressing the hidden driver of test selection: cheating.
Search queries for “how to pass a drug test” number in the millions. Synthetic urine, heating pads, and chemical adulterants constitute a billion-dollar underground industry. Because urine collection requires privacy, even the strictest protocols are vulnerable to sophisticated tampering.
This is where oral fluid gains its most aggressive competitive advantage. Because saliva swabs are collected under direct observation—often right in the HR manager’s office—the opportunity to substitute the sample is entirely eliminated.
But what about the digital rumors? You will find countless internet forums claiming that rinsing with hydrogen peroxide or using specialized neutralizing mouthwashes can defeat an oral swab. Here is the scientific reality: while harsh chemicals might temporarily alter the pH of the mouth, modern high-quality oral swabs and subsequent lab-based LC-MS/MS confirmation testing easily see past these attempts. In fact, attempting to chemically alter oral fluid often triggers an invalid result, prompting an immediate re-test. The adulteration success rate for oral fluid remains statistically at 0%.
Cost-Benefit Analysis of Oral Fluid vs. Urine Programs
Your decision ultimately comes down to aligning your testing method with your industry’s specific operational bottlenecks. Let’s look at three standard models currently succeeding in 2026:
1. The High-Volume Recruitment Model (E.g., Allied Universal)
For massive workforce deployments—like private security, warehousing, and large-scale retail—”speed to hire” is the primary KPI. Sending candidates to an offsite lab for a urine test introduces a 48 to 72-hour delay, during which top candidates may accept other offers.
- The Playbook: Implement in-house, CLIA-waived oral fluid testing. It provides a reliable 99% accuracy rate for recent use, allows for same-day hiring, and completely neutralizes synthetic urine threats.
2. The Regulated Logistics Model (DOT Standard)
Safety-sensitive transportation roles require strict adherence to federal rules.
- The Playbook: A hybrid approach. Use urine testing for comprehensive pre-employment screening to capture historical use, but deploy oral fluid for random, post-accident, or reasonable suspicion testing where immediate, directly observed results are critical and shy bladder delays are unacceptable.
3. The Strict Clinical/Healthcare Model (E.g., Mayo Clinic)
In environments where long-term substance abuse poses an existential risk to patient safety, historical data is more important than rapid onboarding.
- The Playbook: Multi-panel urine cups remain the superior choice. The 7.4x higher overall detection rate for historical use ensures a comprehensive safety net that oral fluid simply cannot provide over a 30-day look-back period.
Making the Right Call for Your Workforce
Transitioning your drug testing policy or selecting the right supplies requires balancing historical detection against operational efficiency. If your primary pain point is candidates faking tests or accepting competitor offers while waiting for lab results, oral fluid provides an unparalleled, heavily observed, rapid-hire solution. If your priority is deep historical screening and maximizing the detection window, multi-panel urine testing remains unmatched in its thoroughness.
Ultimately, a successful drug-free workplace doesn’t rely on just one method—it relies on having consistent access to affordable, premium, FDA-approved testing supplies that your team can trust. Evaluate your current hiring bottlenecks, factor in your industry’s compliance demands, and choose the testing architecture that actively supports your organizational growth.
Frequently Asked Questions (FAQ)
Can a candidate cheat an oral fluid drug test with mouthwash or peroxide?
No. While online myths suggest hydrogen peroxide can neutralize saliva, high-quality, FDA-approved oral swabs capture biological markers that cannot be permanently erased by a quick rinse. Any temporary alteration usually results in an invalid test, mandating immediate observation and re-testing.
Why do some urine tests come back positive for THC while a simultaneous saliva test is negative?
This is the “Metabolite vs. Parent Compound” divide. The candidate likely consumed an edible or smoked several days ago. The active THC (parent compound) has cleared their saliva (usually within 12-24 hours), but the THC-COOH metabolite is still being actively flushed through their urine, which can take weeks.
Is oral fluid testing legally defensible in non-DOT workplaces?
Yes. As long as you are using reliable, FDA-cleared devices and following consistent corporate policy regarding confirmation testing (sending non-negative rapid results to a lab for LC-MS/MS confirmation), oral fluid is legally robust and increasingly favored for its un-cheatable, observed nature.
Which method is more cost-effective?
High-quality multi-panel urine cups can be incredibly affordable (often under $2.00 per unit). However, the total program cost for urine testing is higher when factoring in off-site lab collection fees and the lost productivity of delayed hiring. Oral swabs cost slightly more per unit but drastically reduce administrative overhead and facility fees.

